Making decisions about induction of labour
This toolkit is to support you with choices if you have been offered Induction of Labour (IOL).
It may help you to make informed decisions about your care, in partnership with midwives
and doctors. It’s important for you to understand and be involved in your care planning which
includes discussing the reasons you are offered or recommended an induction.
An induced labour is one that is started artificially (not by itself). Around 3-4 out of 10 women
are induced in the UK. It is your choice whether to have labour induced or not and using this
tool can help you decide and help you ask questions.
Why might I be offered an
induction of labour?
Induction of labour may be offered for a
many different reasons. If you are age 40
or above, you will be offered an earlier
induction of labour. The reason for this is
because there is an increase in the
number of stillbirths in women aged 40
and over. The research is not clear on why
this happens. The research shows the rate
is also higher if you are having your first
baby.
• For women aged 40-43 you will be
offered induction between 39-39+6
weeks pregnant.
• If you are aged 44 or over, we would
usually aim for your baby to be born by
38 weeks.
When considering this choice, you need to
speak to your midwife to see if you have
any other risk factors.
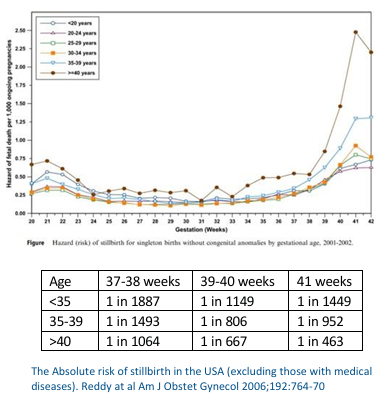
The graph and chart below give you some
statistics from two different research studies.
They show rates of stillbirth as pregnancy
continues and impact of women’s age.
What are the benefits of Induction of Labour?
Usually induction of labour is offered because ending your pregnancy earlier will reduce the
risk of stillbirth as you have a higher risk of this as pregnancy continues.
• Induction of labour after 39 weeks pregnancy does not increase your chances of
caesarean birth, long term problems for your baby or admission to the Neonatal Unit when
compared with continuing your pregnancy.
What are the risks of Induction of Labour?
• The risks of choosing induction will vary depending on your own personal situation. It
may stop a serious infection occurring however it may affect your birth options and limit
your birth place choice.
• You may be recommended more interventions (for example, oxytocin infusion, vaginal
examination, continuous baby (fetal) heart rate monitoring and epidurals) which may limit
your ability to move around).
• There may be a need for an assisted vaginal birth (using forceps or ventouse), with the
associated increased chance of obstetric anal sphincter injury (OASI - third or
fourth-degree perineal tears). The OASI care bundle will be offered to try and reduce this
happening.
• There is a chance the medication used to induce labour could cause hyperstimulation –
this is when the uterus (womb) contracts too frequently or contractions last too long. This
can lead to changes in the baby’s heart rate which could result in the baby being
compromised – we have clear guidelines to follow if there are too many contractions and
we monitor you to ensure your baby is coping with the contractions.
• You may be less likely to be able to use a birth pool.
• An induced labour may be more intense and painful than a natural labour as the
hormones don’t trigger the release of women’s own natural endorphins (which help
relieve pain)
• Your hospital stay may be longer than with a natural labour.
• Sometimes (1 in 100) induction of labour may be unsuccessful and other options would
be discussed with you and the midwives/doctors for a plan to be made together.
• Your highest chance of a vaginal birth is if it starts naturally (by itself) and you birth on a
Midwife-Led Unit near Delivery Suite – speak to your consultant midwife to explore this
option.
What are the alternatives?
• You have the option of waiting longer to see if you labour starts naturally.
• You could choose to be induced at a later date.
• If you would like to discuss any other alternative options, please let the midwives know
about this and they will arrange for an appointment with a doctor or consultant midwife to
ensure there is a clear plan with you.
What happens now?
• It is important to make a choice that is right for you.
• Try using the tool below to help you make a decision that is right for you and your baby.
• The midwives will book your induction of labour if this is what you choose and give you a
time to attend the Delivery Suite.
• If you choose to wait for your labour to start or wait longer
for your induction of labour, extra monitoring of you and
your baby will be offered. You should also discuss your
plans with the obstetric doctors if you wish to wait
longer. This is due to your risk increasing if you
continue your pregnancy. Extra monitoring cannot
guarantee the wellbeing of your baby, but it may pick
up concerns at the point of the monitoring.
Think about...
What are the benefits?
What are the risks?
What are the alternatives?
What does your intuition or your gut feeling tell you?
What happens if we do nothing for now? Can we wait and take some time to think?
Second opinion...do I need one?
Further information
The Induction of Labour Information for
Birthing People and their families which
gives further information on induction of
labour
• including
• process
• risks
• membrane
sweep
• stages of
induction

